Top 10 Most-Feared Diagnostic Errors for Trainees in Pediatric Neuroradiology Emergencies
Survey of senior radiology residents revealed on-call potential errors most challenging to trainees

Shortened image acquisition times and greater MR availability are allowing even the youngest patients to undergo imaging, which is especially helpful in the emergency department, where infants and young children present with life-threatening conditions. However, for radiologists in training, interpreting the imaging studies of pediatric patients presents unique challenges.
“Pediatric neuroradiology is a subspecialty within a subspecialty,” said Agustín Cárdenas, MD, clinical assistant professor of pediatric neuroradiology at the Hospital Universitario Doce de Octubre, in Madrid, and the Children’s Hospital of Alabama/University of Alabama at Birmingham. “So many trainees and attending radiologists are fearful whenever they see a CT of a two-year-old or an MRI of a five-year-old because the pediatric brain, pathology and myelination are different, and the differential diagnosis changes.”
Throughout his career, Dr. Cárdenas said he has noticed a pattern of common fears among trainees when interpreting pediatric neuroradiology CT and MRI studies.
“There are differences in the appearance of pathophysiologic conditions and disease in pediatric patients compared to adults,” he said. “Limited exposure during training contributes to the complexity of interpreting these imaging studies, especially in the emergency setting.”
To better understand these challenges, Dr. Cárdenas and a team of researchers surveyed 35 senior radiology residents in 22 different residency programs in the U.S. and Europe to identify their most feared diagnostic errors when on call. Once the top 10 potential errors were identified, the researchers generated practical tips and tricks to help prevent them.
“Trainees are regularly exposed to adult brains, making them more familiar with what is considered ‘normal’,” he said. “However, acute emergency findings can be easy for trainees to overlook, especially when they are accustomed to the appearance of a typical 50-year-old brain.”
Breaking Down the Top Five
Ranking No. 1 in the survey as the most dreaded potential error was the detection of early cerebral edema. Nearly all survey respondents feared missing this diagnosis.
“Not only are the initial findings subtle, but many trainees are unfamiliar with cerebrospinal fluid (CSF) spaces in children,” he said. “Early edema can be very difficult to see, and there are grave implications for missing it.”
To prevent the condition from being missed, the researchers suggested becoming familiar with the normal appearance of basal cisterns. “Basal cisterns and CSF spaces along convexities are your friend,” Dr. Cárdenas said.
Coming in at No. 2 was detecting dural sinus thrombosis with non-contrast CT. Missing this relatively uncommon condition was feared by 73% of survey respondents.
According to Dr. Cárdenas, vague symptoms, dural sinuses that appear normal, and a relatively high hematocrit level (typical in neonates) make this diagnosis challenging. “Clinically, dural sinus thrombosis can be very silent and subtle,” he said.
Prevention tips include conducting a quantitative analysis and adjusting for hematocrit levels.
Correctly distinguishing between retropharyngeal edema and early abscess was No. 3 on the list, with 63% of senior residents fearing a potential error in such a case. Dr. Cárdenas said looking for the enhancement pattern and mass effect is helpful for trainees faced with answering this question.
More than half of the survey respondents considered detecting early shunt failure challenging, giving it a No. 4 ranking. In addition to always comparing with prior images when available, Dr. Cárdenas said trainees should look for sulcal effacement near the vertex. “Early shunt dysfunction can be easily missed, particularly in patients with developmental delays,” he said.
At No. 5—feared by 56% of respondents—was incorrectly diagnosing a craniocervical junction (CCJ) fracture. “Radiology trainees often overcall fractures because they lack familiarity with the imaging appearance and timing of the normal ossification centers of C1 and C2 on CT,” he said.
Learning more about the imaging appearance of normally developing ossification centers will help trainees accurately identify fractures.
“The craniocervical junction in pediatric patients is more flexible and has more laxity than adults,” he said. “Fractures are rare in infants and young children, but MRI may help assess ligamentous injuries.”
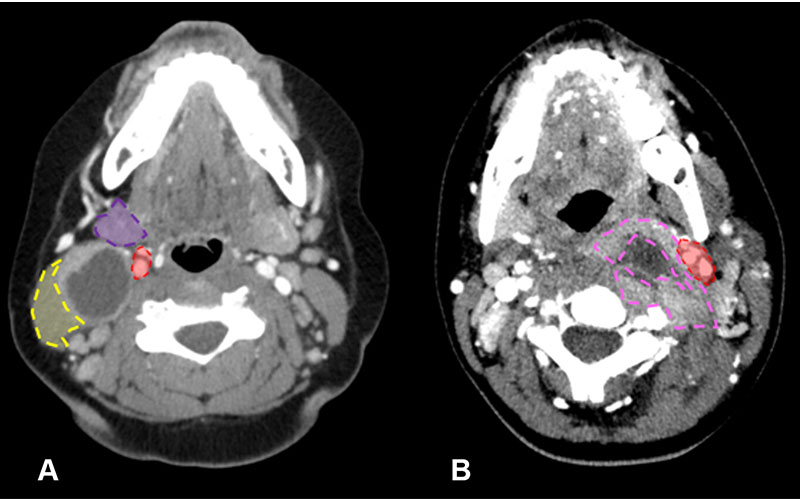
Distinction between branchial cleft cyst and retropharyngeal abscess in two pediatric patients who visited the emergency department due to neck pain and swelling. (A) Axial CT image of the neck in a 10-year-old girl shows typical imaging characteristics strongly indicative of a branchial cleft cyst. This is evident from the lesion location posterior to the submandibular gland (purple shaded area), lateral to the carotid space (red shaded area), and anteromedial to the sternocleidomastoid muscle (yellow shaded area). (B) Axial CT image in a 12-year-old girl conversely shows features that align more with a retropharyngeal abscess. This is characterized by an irregular and thick enhancing wall (pink dashed outline), accompanied by surrounding fat stranding and edema. Notably, this lesion is situated medially to the carotid space (red shaded area). (See slide 35 in the accompanying presentation.)
https://doi.org/10.1148/rg.240123 ©RSNA 2024
Targeting Training To Increase Skill, Confidence
Rounding out the list of most feared errors or misses were:
- Calvarial fractures versus sutures
- Branchial cleft cyst versus retropharyngeal abscess
- Time estimation of heterogeneous subdural hematomas (33%)
- Porencephalic cyst versus ventriculomegaly (30%)
- Detection of early orbital cellulitis (3%)
For Dr. Cárdenas, the low ranking of estimating the time of subdural hematomas was worrying. “I'm concerned that only 33% of the residents are fearful of estimating the time of heterogeneous subdural hematomas,” he said. “Over past decades, we have overestimated our ability to do this. We must be more cautious and refrain from using the terms ‘acute’ and ‘chronic’.”
In response to the survey results, the researchers curated a list of bibliographic resources to help trainees feel more confident when reading pediatric imaging studies.
“Instead of recommending hundreds of papers, we recommend 10-15 that trainees can read to feel more comfortable when facing these complex cases,” he said. “When interpreting pediatric neuroimaging, it’s most important for radiologists to learn from normal cases and build and develop an ‘internal normal’ template.”
Editor's Note: Readers can access the bibliography of articles recommended to assist with pediatric neuroimaging by visiting the RadioGraphics article and clicking on the Full Digital Presentation of this education exhibit.
For More Information
Access the RadioGraphics article, “Top 10 Most-feared Diagnostic Errors for Radiology Trainees in Pediatric Neuroradiology Emergencies.”
Read previous RSNA News stories on pediatric imaging:
- Pediatric Head and Neck Disease Awareness Essential for Accurate Diagnosis
- Understanding the Imaging Spectrum of non-Hodgkin Lymphoma in Children, Adolescents and Young Adults
- Persistent Pulmonary Manifestations in Children Following COVID-19